Porphyromonas gingivalis (Pg) is a key driver of severe periodontitis through the release of toxins called gingipains. Gingipains subvert the host immune responses, protecting Pg from immune attack, whilst corrupting immune cells to drive inflammation.
Due to the chronic nature of disease, the inflammatory response leads to progressive tissue damage, resulting in loss of the bone and ligaments that support the tooth. Without treatment, ultimately, this leads to tooth loss.
The Impact of Severe Periodontal Disease on Patients.
Severe periodontitis is a debilitating gum disease. It affects people across all income groups, but its prevalence is highest in smokers and diabetics. Those in lower socioeconomic demographics are more likely to experience severe symptoms due to lack of access to appropriate and affordable care.
The disease damages periodontal soft tissue and alveolar bone that supports the teeth, which can ultimately lead to affected teeth falling out.
Severe periodontitis not only causes physical pain but is also associated with an increased risk of anxiety disorder (by 35%) and depression (by 70%).
The World Health Organisation estimates there are more than one billion cases of severe periodontal disease worldwide (19% of all adults).

Current treatments
There is no cure for periodontitis. Current treatments, such as scaling and root planning, that attempt to slow down disease progression, are painful, expensive and require repeated application. Currently available adjunct therapies provide very modest and short-lived benefit.
Why will targeting gingipains work better than other approaches?
Periodontitis is a chronic inflammatory disease driven by the gingipain toxins of P. gingivalis (Pg). In severe periodontitis gingipains are released at high levels and penetrate the surrounding tissues. The gingipains are potent proteolytic enzymes able to damage surrounding tissues and dysregulate host immune responses, corrupting them to drive chronic inflammation. This has been shown to be a key driver of severe periodontitis.
By neutralising gingipains, we intend to remove the driver of chronic inflammation. We aim to restore the functional immune responses in patients with advanced and refractory disease. This approach has been shown to be successful in both animal challenge models and natural disease setting.
Chronic diseases linked with Porphyromonas gingivalis
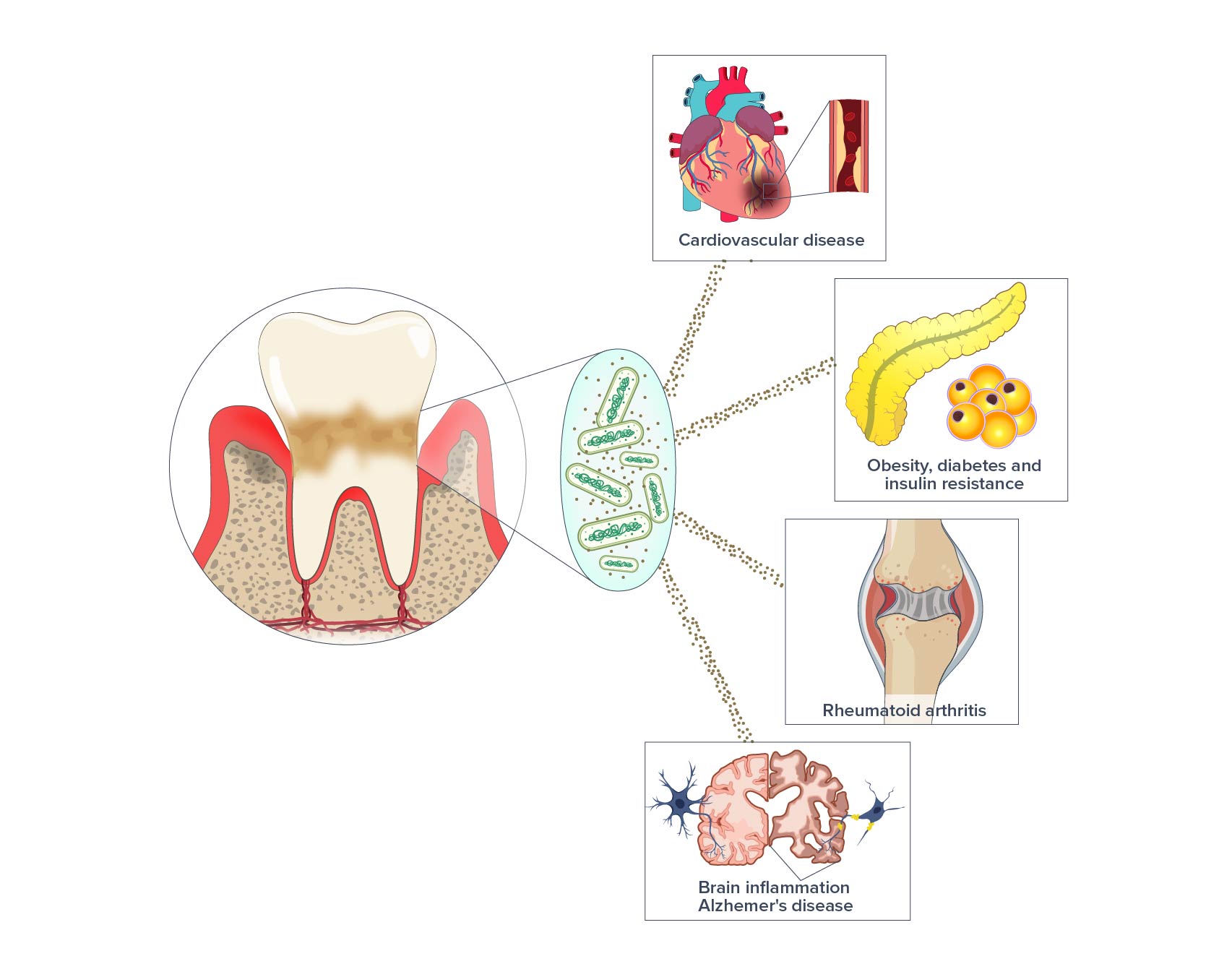
P. gingivalis (Pg) is not only associated with severe periodontitis. There is a growing body of evidence identifying potential links between Pg and other diseases including Alzheimer’s disease, diabetes, cardio-vascular diseases, rheumatoid arthritis, and certain cancers. The chronic nature of periodontitis can expose the body to the gingipain toxins over many years and even decades, hence the connection to these systemic chronic conditions. Furthermore, the ongoing inflammatory response in the tissues of the mouth can spill over into the systemic circulation, leading to a heightened immune response throughout the body.
Alzheimer’s Disease
P. gingivalis releases toxins called gingipains. Research has found gingipains in the brains of patients with Alzheimer’s disease, with their levels correlating with disease pathology.
In a recent clinical study, a drug targeting the gingipains resulted in a significant slowing down of the cognitive decline in Alzheimer’s disease patients with oral P. gingivalis infection.
If you would like to learn more about our upcoming Phase I safety study in early Alzheimer’s disease (AD) in Melbourne, please contact us via the form at the bottom of the page.
Diabetes
P. gingivalis (Pg) has long been associated as a risk factor with diabetes. The gingipains produced by Pg contribute to insulin resistance by disrupting insulin signalling pathways.
Heart Disease
P. gingivalis, has been found in lesions of the cardiovascular system and shown to promote the development of atherosclerosis and disrupt endothelial integrity.